Nuvo Improves Pregnancy Care - Even For Women Living Through A War

Forbes article highlighting Nuvo's impact on patients and providers around the world... "Nuvo’s FDA-cleared INVU™ solution provides that "care everywhere" and allows for non-invasive maternal heart rate, fetal heart rate, and uterine activity monitoring - without requiring a visit to a hospital or doctor’s office. Instead, during their clinician-prescribed timeframes, women can apply INVU™ while they’re at home or even at work, as Dr. Platt notes. The real-time data from these monitoring sessions allows their healthcare providers to assess the condition of the fetus and the urgency for delivery - especially in, though not limited to, women with high-risk conditions for whom American College of Obstetricians and Gynecologists (ACOG) guidelines recommend regular fetal monitoring. These conditions can include medical complications that can lead to abnormal fetal growth, diabetes, stillbirth, and more."
This article was originally published by Forbes here.
By Eva Epker, Forbes Contributor
“How is it possible that, in the 21st century, you can’t monitor a baby outside of a hospital?” In 2014, Oren Oz and Laurence Klein asked that very question. At the time, Mr. Oz’s wife was 37 weeks pregnant with the couple’s third child. When she went for her pre-labor and delivery ultrasound, the doctor told her that the baby was in distress and recommended an immediate emergency C-section.
Emergency Cesarean sections (C-sections) – which, despite the name, don’t refer to emergencies exclusively but rather to unplanned C-sections generally – are not unusual. In fact, C-sections, both emergency and elective, are the most common surgeries performed every year in the United States and about 17 births out of every 100 are through emergency C-sections.
However, C-sections do carry risks. About 15% of emergency C-sections have complications, such as infections, lacerations, and bleeding for the mother and neonatal respiratory distress for the baby. The maternal morality rate, the mother’s recovery time, and the costs additionally increase with C-sections compared to vaginal births. A 2022 analysis found that vaginal births in the United States cost an average of $14,768 while C-sections, both emergency and elective, average $26,280. For those with insurance, the out-of-pocket costs are $2,655 and $3,214 respectively.
Nearly ten years ago, Oren Oz and his wife decided not to undergo an emergency C-section Instead, she stayed at the hospital for 24/7 monitoring, gave birth vaginally as planned, and both she and the baby were healthy. But that medical scare - and the anxiety and hospital stay that followed - led to the founding of Nuvo Cares, which has developed a self-administered solution that enables OB clinicians and their patients to conduct medically-necessary fetal monitoring remotely: where it fits into the patients’ lives. “If no one has been able to monitor pregnancy more easily and frequently, [we as a society] don’t have data at scale on pregnancy. It’s a black box,” says Nuvo investor Laurence “Larry” Klein. The mission of Nuvo is to collect this data and to transform pregnancy for the next several generations, and, as Mr. Klein emphasizes, there is “no compromise” on that mission.
Childbirth, after all, is the single most-common cause of hospital admission in the United States and accounts for an estimated four out of every five dollars spent on maternal-newborn health care. And yet, the cost of childbirth is increasing (it jumped 22% from 2017 to 2021 alone), maternal mortality is increasing (doubling over the course of 20 years and most affecting Black, Native Alaskan, and Native American women), and the number of C-sections is rising (increasing from 5.5% in 1970 to the current 32.1%). A 2022 study found that each year of “increasing maternal age [increases] the odds of emergency [C-sections] by 6%” – and the average age of first-time mothers has been increasing steadily: from 21.4 in 1970 to 24.9 in 2000 to 27.3 years old today.
Regular OB/GYN appointments can help mitigate some of these risks. But almost half of all counties in the United States lack practicing OB/GYNs, leaving 8.2% of all women - or more than 10 million women - with little to no access to OB/GYNs and to tools, tests, and technologies such as ultrasounds. During their pregnancy, women will have at least two ultrasounds but will sometimes have more, depending on the risk level of the pregnancy. The ultrasounds confirm the number of embryos, show the baby’s sex, calculate the baby’s due date, and, as the pregnancy progresses, check for any abnormalities, such as in the baby’s heart rate or in its developing brain, limbs, organ, spine, and more.
Even if women do have access to the needed specialists and monitoring tools, they need to be physically in a doctor’s office or hospital to reap the benefits of those services: a privilege not all women can afford. A low-wage or hourly worker, for instance, may not be able to afford time off for OB/GYN appointments, and women generally - and Black and Latina women specifically - are disproportionately likely to be low-wage workers than (white) men are.
In contrast, Nuvo can help “provide care everywhere”: an underlying premise that is simple and yet is simultaneously a major advance in healthcare, according to Dr. Lawrence “Larry” D. Platt MD, who is one of the foremost maternal fetal medicine (MFM) specialists in the United States. Widely acclaimed, accoladed, and published, his affiliations include the Center for Fetal Medicine and Women's Ultrasound, the Department of Obstetrics and Gynecology at the David Geffen School of Medicine at UCLA, and Nuvo’s Advisory Board.
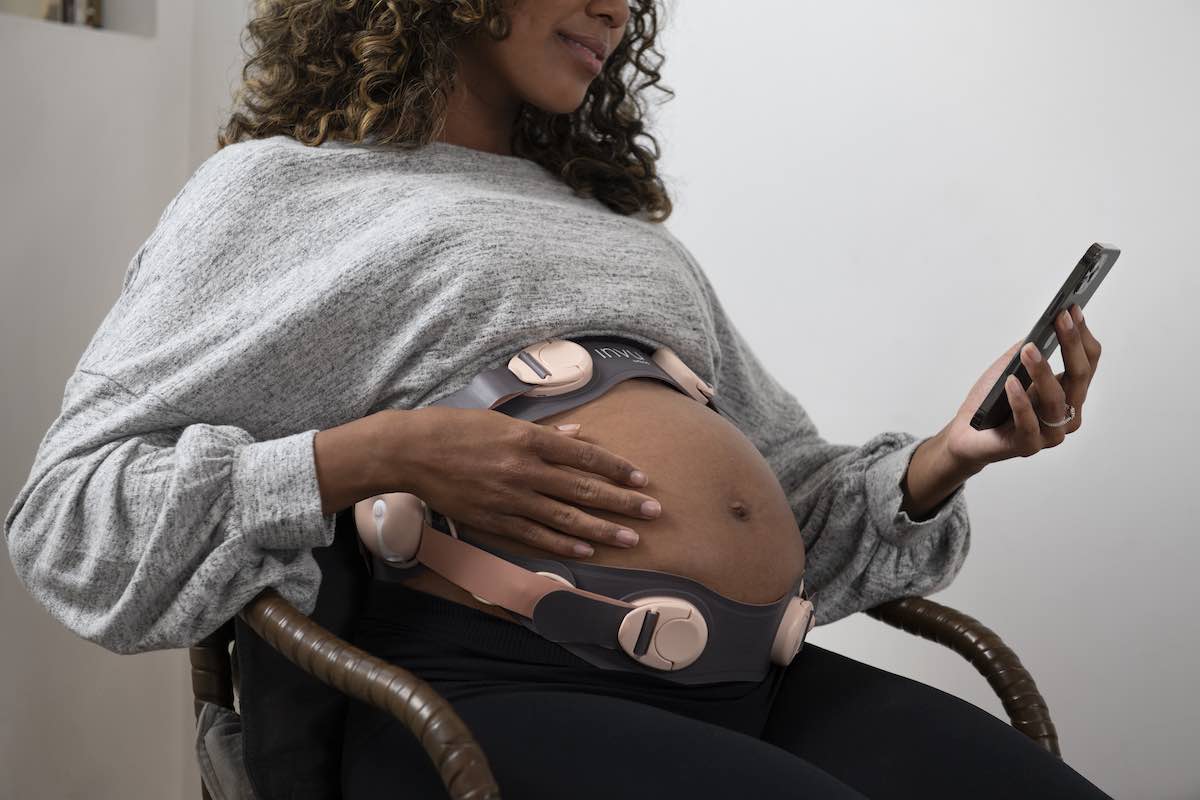
Nuvo’s FDA-cleared INVU™ solution provides that "care everywhere" and allows for non-invasive maternal heart rate, fetal heart rate, and uterine activity monitoring - without requiring a visit to a hospital or doctor’s office. Instead, during their clinician-prescribed timeframes, women can apply INVU™ while they’re at home or even at work, as Dr. Platt notes. The real-time data from these monitoring sessions allows their healthcare providers to assess the condition of the fetus and the urgency for delivery - especially in, though not limited to, women with high-risk conditions for whom American College of Obstetricians and Gynecologists (ACOG) guidelines recommend regular fetal monitoring. These conditions can include medical complications that can lead to abnormal fetal growth, diabetes, stillbirth, and more.
For example, women who have previously had a stillbirth have higher risks of having pregnancy complications and of having another stillbirth – and are, therefore, tested more frequently, require more monitoring and come to the hospital more frequently out of concern – than women who have had a live birth. They are also five times more likely to develop anxiety, more than four times more likely to have post-traumatic stress disorder, and two times more likely to have depression than women who have had a live birth. With INVU™, women can have a monitored session with their healthcare provider in the convenience of their home, office, and daily life rather than having to leave their work, leave their children, and/or generally go out of their way to a hospital. But they still have the benefits of remaining connected to their healthcare provider and having their pregnancy monitored – including tracking fetal movement, which one of the most inexpensive ways to prevent stillbirth – just as they would in that healthcare setting. “In this process [INVU™] alleviates anxiety in that one group of pregnant women, not to mention many others,” Dr. Platt concludes.
That INVU™ uses different sensor technologies (ECG and acoustic sensors) than the ones used in traditional pregnancy monitors in hospitals and doctors’ offices allows it both to be an additional source of data and monitoring to ultrasounds and to provide unique physiological insights into the health of the mother and baby. As long as women are wearing their device, their healthcare providers can interact with and evaluate them at any time or place.
In turn, INVU™ can provide information and achieve milestones that otherwise may not have been possible – much less appreciated by, accepted by, and advantageous for providers and patients – such as those seen in Israel’s Sheba Hospital. Sheba Hospital, also known as Tel HaShomer Hospital, is the largest hospital in Israel, the largest medical center in the Middle East, and one of the top 10 best hospitals in the world. In addition, it cares for more injuries caused by the war than all of Israel’s other hospitals combined.
After the attack on Israel on October 7, 2023, Sheba Hospital moved some of its patients out of the hospital to free up space and resources for those injured during the war. One of the wards it moved was for geriatrics. Another was for high-risk pregnancies: pregnant women who, due to medical complications, diabetes, a previous stillbirth or another reason entirely, were mandated to be in the hospital for continuous monitoring. Sheba Hospital sent those patients home and used INVU™ to monitor them instead: a decision that, as Mr. Klein explains, would have been impossible if Sheba Hospital hadn’t believed that Nuvo could provide medical care equivalent to that of the hospital itself. Now, several months into the war, Mr. Klein calls the operation a “phenomenal success”: groundbreaking both because of the scale of the operation and because the involved pregnant women maintained, or even improved, their health, despite this move from hospital to home. In one case, a mother at Sheba whose doctors thought she would give birth at 34 weeks didn’t give birth until 37 weeks: out of the premature birth range and to the benefit of the baby.
Nuvo’s success in high-risk mothers in Israel, as Mr. Klein observes, is representative of the benefits that Nuvo can provide, even in places that are not war-struck. “I believe that healthcare will change fundamentally when the patient says, ‘I want this,’” he says. Dr. Platt agrees, calling Nuvo “one of those innovations that will change care”. Nuvo’s INVU™ solution can be that care-changing, transformative tool that patients “want”. It can help address the issues of accessibility, cost, inequality, and risk that come with pregnancies without requiring only in-hospital monitoring: the same thesis that inspired the founding of Nuvo nearly ten years ago.